C-Section
A cesarean section is a birth where the delivery occurs through an incision made in the mother’s abdomen. Complications during birth may lead a doctor to recommend an emergency C-section for their patient when there are delays in the labor process and the fetus begins to experience distress.
Home > Delivery Complications > C-Section
- Last Updated Date: March 31, 2026
Navigate This Page
- What is a C-section?
- What are some reasons women need C-sections?
- What is the difference between vaginal birth and a C-section?
- What happens during a C-section??
- What are the risks of a C-section to the woman?
- What are the risks of a C-section for the baby?
- Is a C-section painful?
- How long does C-section recovery take?
- In Conclusion
According to data from the Centers for Disease Control and Prevention (CDC), almost 32 percent of births in the United States occur via cesarean section each year. Out of more than 3.9 million births annually, approximately 1.4 million babies are delivered by C-section.
Undergoing a C-section is a relatively safe procedure; however, complications may occur in some cases. The operation is considered major surgery, but some women decide to undergo the procedure as elective surgery. Data from the World Health Organization (WHO) indicates that worldwide cesarean section rates have increased by 14 percent since 1990.
What is a C-section?
A cesarean section, or C-section, is a type of surgery where a doctor makes an incision into a woman’s abdomen and womb to deliver a baby. The operation was once considered a last resort for women and babies in mortal danger during birth, but now the procedure occurs millions of times a year, and health-care providers today consider it very safe.
The name of the procedure comes from the Latin word “caesus,” which means “to cut.” In a grisly practice common in ancient Rome, mothers who died while pregnant were given rudimentary cesarean sections to remove their babies because religious practices at the time prohibited the burial of pregnant women.
Cesarean delivery as we know it today was developed around 100 years ago when general anesthesia became widely available and doctors were more aware of proper antiseptic procedures for surgery in the operating room. By the 1940s, C-sections became increasingly popular because of their increased safety and the opportunity for a doctor to maintain the baby’s health as well as the mother’s life.
What are some reasons women need C-sections?
Some women elect to have a C-section before they go into labor because their baby is large, the mother has a transmissible condition like HIV or herpes, or the pregnancy is a multiple birth with twins or triplets. Some medical conditions like diabetes or high blood pressure may indicate the need for a C-section.
There are also emergency cesarean sections that occur at the time of labor because of problems like a breech presentation, which is where the baby’s buttocks or feet would be born first rather than the head. A placenta previa, where the placenta blocks the birth canal, may also require that the vaginal birth switch to a C-section.
When a woman’s cervix doesn’t open enough for labor to progress, a doctor may need to perform a C-section. Issues with the umbilical cord getting pinched or an abnormal heart rate may also indicate an emergency C-section is needed to save the baby and the mother.
Many women who have a cesarean birth must undergo C-sections when they get pregnant again. Although some women want a VBAC or vaginal birth after a cesarean section, vaginal deliveries generally come with added risks after a woman has already undergone a C-section, so one C-section sometimes leads to repeat C-sections during future pregnancies.
- Last Updated Date: March 31, 2026
"*" indicates required fields
What is the difference between vaginal birth and a C-section?
A C-section requires some preparation that isn’t necessary with a vaginal birth. The woman undergoing the procedure will need an IV for antibiotics and fluids and may also require general anesthesia from an anesthesiologist. Some women who undergo C-sections will receive an epidural or spinal block, which means they’ll remain awake during the procedure.
With a vaginal birth, a woman might receive an epidural, which is a regional anesthesia that will reduce pain during vaginal birth, but she won’t undergo general anesthesia unless the doctor determines that an emergency C-section is required because of maternal or fetal distress.
Another step the C-section health-care team will take that is different from a vaginal birth procedure is the insertion of a catheter into the woman’s urethra, which will drain the bladder and reduce the likelihood of infection. The surgeon’s team must also wash the woman’s abdomen before beginning the surgical procedure because of an increased risk of infection due to the abdominal cuts.
What happens during a C-section?
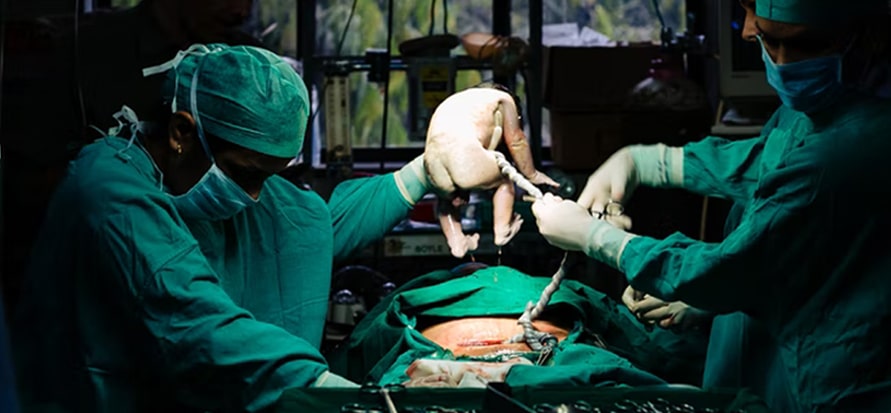
During a C-section, the surgeon will separate a woman’s abdominal muscles to gain access to her uterus. The doctor will make a horizontal incision or vertical cut in the wall of the uterus, after which the doctor will deliver the baby through the incision.
After successful delivery, the doctor will cut the umbilical cord and remove the placenta. The doctor will then close the abdominal incisions. The uterine incision is closed with stitches that will dissolve in the woman’s body, and the abdominal skin is closed with staples or stitches. Incredibly, a C-section only takes about 20 minutes once the surgeon makes the first incision.
What are the risks of a C-section to the woman?
A C-section isn’t without risks, even when the procedure must occur to save the life of a fetus or pregnant woman. As with any surgical procedure, a C-section may cause an infection at the wound site. Signs of infection include redness, pain, swelling, and unexplained discharge at the incision.
An infection may also occur within the body during postpartum recovery. An infection of the womb may cause symptoms like fever, pain in the stomach area, vaginal bleeding, and discharge. Significant blood loss may occur in rare circumstances, which could require the woman to undergo a blood transfusion.
Another risk is the formation of a blood clot in the leg, or deep vein thrombosis (DVT). This condition may cause pain and swelling and become life-threatening if the clot travels to the lungs and causes a pulmonary embolism.
In rare cases, a woman may experience damage to organs in proximity to the uterus. Damage to the tubes that connect the kidneys to the bladder as well as damage to the bladder may occur and require that the woman undergo further surgery.
According to the UK’s National Health Service (NHS), some risks also exist for future pregnancies. A woman who becomes pregnant again after having a C-section is at an increased risk for stillbirth as well as having a scar on the womb open during pregnancy.
Some women experience a complication where the placenta attaches abnormally to the wall of the womb, which may make it difficult to deliver the placenta in future pregnancies. A uterine rupture may also occur in a future pregnancy in some women who opt for a VBAC.
What are the risks of a C-section for the baby?
Although a C-section may save a baby’s life, the procedure isn’t entirely without risks for the fetus. A common risk is a cut to the baby’s skin, which may occur accidentally when the surgeon makes an incision in the uterine wall. Fortunately, these cuts aren’t usually severe and quickly heal without any complications.
A baby may also experience breathing problems during a surgical delivery that will require close monitoring of the baby’s vital signs for a few days post-delivery. Breathing difficulties most often occur when babies are delivered before their due date or before 39 weeks of pregnancy.
Postpartum depression is a risk for all women who give birth, and some women may benefit from mental health assistance when they experience depression beyond the date of their first postpartum appointment.
Is a C-section painful?
A woman who undergoes a C-section shouldn’t feel any pain during the procedure. Anesthesia should prevent it; however, some women report feeling pressure or pulling during the procedure when they undergo regional anesthesia.
The pain and risks of a C-section aren’t too different from what a woman might experience with vaginal birth; however, a C-section will usually require that a woman remains in the hospital for two to four days, while some women who have vaginal births will leave the hospital the same day they give birth.
One of the greatest differences in the pain of a C-section versus a vaginal birth is that a C-section may take much longer for a full recovery. A woman may experience pain at the incision site for several weeks after the surgery, and other women may experience urinary incontinence because of a weakening of their pelvic floor muscles.
How long does C-section recovery take?
Recovering from a C-section often means getting enough rest, managing pain with over-the-counter medications, and returning to the doctor when pain doesn’t subside or when the woman suspects an infection.
Some women may have problems with constipation during their recovery because they spend a lot of time lying down due to their surgical incisions. A woman’s hormones may change dramatically after giving birth, and these changes can create even more risks for constipation. Doctors will usually recommend that women keep their water intake high to aid recovery from constipation and to ensure better wound healing in the months after a C-section.
For some women, full recovery might take months even if they don’t experience complications after surgery. Some women may experience difficulties breastfeeding after a C-section, and it’s important for women to ask for help when they have trouble nursing. A breastfeeding cushion or a comfortable chair can help.
In Conclusion
The field of obstetrics has seen incredible advancement in reducing maternal and infant mortality in the last century, due in large part to the safe delivery of babies via cesarean section. The procedure is not without risks, and dire complications may occur in some cases, but a health-care professional may recommend the procedure when there is a high likelihood of complications from vaginal birth.
Written by:
Birth Injury Center Team
The Birth Injury Center aims to create informational web content and guides to help women and their families seeking support and guidance for birth injuries caused by medical negligence. All of the content published across The Birth Injury Center website has been thoroughly investigated and approved by medical expert Natalie Speer, RNC-OB.

