Cooling Therapy Treatment for HIE
Hypoxic-ischemic encephalopathy (HIE) is a birth complication caused by restricted blood flow and oxygen to the infant’s brain. Because brain tissue requires constant energy, even brief periods of deprivation can cause permanent brain damage.
Home > HIE (Hypoxic-Ischemic Encephalopathy) > Cooling Therapy Treatment for HIE
- Last Updated Date: March 30, 2026
Navigate This Page
- What Is Cooling Therapy For HIE?
- How Does Cooling Therapy For HIE Work?
- When Should A Baby With HIE Be Treated Using Cooling Therapy?
- When Shouldn’t Hypothermia Treatment For HIE Be Used?
- Re-Warming For Babies After a Cooling Treatment for HIE
- What Happens After Hypothermia Treatment for HIE?
- Benefits of Cooling Treatments for HIE
- Risks of Cooling Treatments for HIE
HIE, also known as birth asphyxia, perinatal asphyxia, and neonatal encephalopathy, is a serious condition and requires swift diagnosis and treatment. In the past, treatment options were limited. Experimental new treatments such as cooling therapy are now being tested in the hope of altering an infant’s prognosis after HIE occurs.
After an HIE diagnosis, 40% to 60% of infants either do not survive past two years of age or suffer a severe intellectual disability, such as mental retardation, epilepsy, or cerebral palsy. Cooling therapy treatment may reduce this mortality rate and the severity of brain damage caused by HIE.
What Is Cooling Therapy For HIE?
Cooling therapy is a treatment option that medical teams are exploring as a solution to HIE. The therapy induces therapeutic hypothermia, or a lowered body temperature, in the infant. The use of this therapy has been shown to reduce the likelihood and severity of permanent brain damage in newborns with HIE.


Although there is strong evidence to show that cooling therapy is effective, scientists are still working to discover the mechanisms behind why this therapy works. The current theory is that it works by lowering the metabolic rate of cells.
Brain damage following an injury to the brain doesn’t just occur during the injury itself. Rather, the body’s response to the injury causes additional damage. By slowing down the rate at which cells function, the body’s response is also slowed. This allows brain cells to recover with less damage, which can improve long-term neurodevelopmental outcomes.
Cooling therapy must be administered within six hours following birth. Treatment options include selective head cooling or whole-body cooling. The infant’s body temperature is cooled to 92.3 to 94.1 degrees Fahrenheit for 72 hours.
This therapy is intended for infants with moderate or stage 2 HIE. Research results have shown less efficacy when treating severe (stage 3) HIE, although the treatment may be tried for these babies anyway. Hypothermia treatment is intended for infants carried to full-term, and research studies have shown no treatment benefit to infants born earlier than 36 weeks
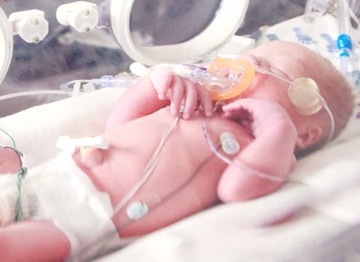
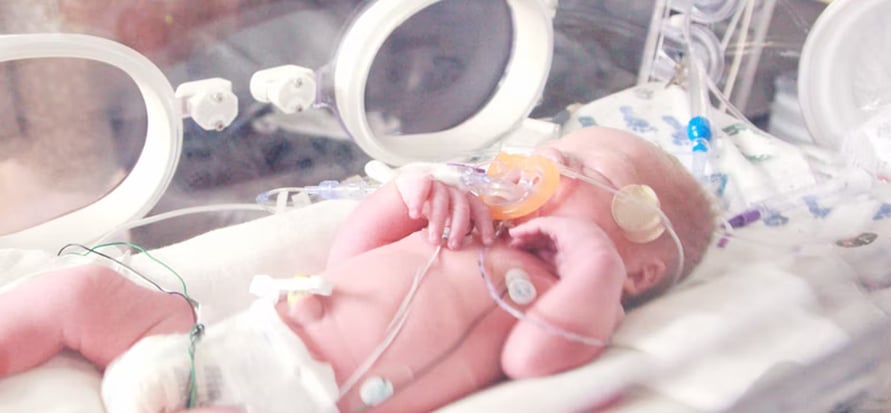
How Does Cooling Therapy For HIE Work?
Cooling methods may vary, but the basic guidelines for temperatures and timing increments must be followed carefully. Cooling therapy relies upon the active cooling of the baby’s entire body, but in some cases, it may be necessary to use passive cooling in conjunction with active cooling.
- Last Updated Date: March 30, 2026
"*" indicates required fields
Passive Cooling
Passive cooling is an additional intervention measure used to prepare the baby for active cooling. Passive cooling is used only in situations when the birth takes place at a location where cooling therapy cannot be immediately initiated. For passive cooling, medical professionals place the newborn in an environment that lacks any form of heat source, and they regularly check and record the newborn’s body temperature through a rectal or axillary (armpit) thermometer.
Sometimes, an infant arrives at the medical facility where cooling therapy will take place at or near the end of the crucial six-hour window. In these situations, passive cooling may be initiated by medical professionals to help the infant’s body temperature drop more quickly. Passive cooling prepares the infant for active cooling upon arrival at a neonatal intensive care unit.
Active Cooling
The active cooling process varies by hospital. The standard for active cooling includes:
- Treatment initiated within six hours of birth
- Treatment duration of 72 hours
- Continuous monitoring of core body temperature
- Body temperature kept between 92.3 and 94.1 degrees Fahrenheit
Cool packs at 50 degrees Fahrenheit are wrapped in cotton and applied to the infant’s body. These cool packs should be cold but never frozen and should never come into direct contact with the infant’s skin.
Once the infant’s core body temperature reaches between 93.2 and 95.5 degrees Fahrenheit, cooling should be reduced to one cool pack across the chest.
If body temperature drops below 93.2 degrees Fahrenheit, all cool packs should be removed. If the infant’s body temperature continues to drop, a warmer can be used to raise the temperature back to the desired range for cooling therapy.
Active cooling aims to continually monitor core body temperature with a rectal temperature probe and adjust the application of cold packs to maintain the target temperature range.
Ideally, the infant’s body temperature should reach the desired range within the first hour, and then cooling treatments should be maintained for 72 hours. Once complete, the infant should be returned to a standard body temperature over a minimum four-hour period.
Different hospitals may use different neonatal cooling methods, but they must follow temperature guidelines. Some facilities may opt for a cooling blanket or an alternative cooling device.
A cooling blanket involves laying the infant on a waterproof blanket while cold water circulates beneath it. A fan may be used in conjunction with other cooling methods. Sometimes cooling devices are applied under the head in addition to the shoulders and chest.
When Should A Baby With HIE Be Treated Using Cooling Therapy?
Cooling therapy is appropriate for some instances of neonatal hypoxic ischemic encephalopathy. Candidates for treatment should be full-term infants who display signs of HIE.
Hypoxia is identified when an infant meets at least two of the following physiological criteria:
- An Apgar score of 5 or less at 10 minutes after birth
- Need for ventilation or ongoing resuscitation at 10 minutes
- Signs of blood gas abnormalities within the first hour
Additionally, health care professionals can diagnose HIE through imaging technology, including magnetic resonance imaging (MRI), computerized tomography (CT), and ultrasound (US).
Once these criteria identify hypoxia, an infant should also show at least one of the following neurological criteria:
- Seizure activity
- Evidence of encephalopathy via amplitude-integrated EEG (a-EEG)
- Physical examination suggesting moderate to severe HIE
Newborn babies who meet these criteria are most likely to benefit from the therapeutic effects of hypothermia and make the best candidates for cooling treatment for HIE.
When Shouldn't Hypothermia Treatment For HIE Be Used?
Hypothermia treatment is not without risks, and only infants who meet the above criteria should undergo this form of treatment. There are many situations in which hypothermia treatment appears to be ineffective or the infant does not safely qualify for treatment.
The following criteria indicate instances in which infants should not receive hypothermia treatment:
Failure to meet physiological and neurological criteria
Premature babies born earlier than 36 weeks
Birth weight of less than 4.4 lbs
More than six hours have passed since the time of birth
Coagulopathy (impaired blood clot formation) is suspected
Life-threatening cardiovascular or respiratory abnormalities
Major congenital malformations exist
Imperforate anus (missing or blocked opening to the anus)
Suspicion of neuromuscular disorder
Lethal chromosomal anomaly
Infant death is inevitable
Recent studies show that therapeutic hypothermia has a better chance of success for infants with moderate encephalopathy. Treatment can be initiated in severe cases, but cooling treatment appears to be less effective when the type of brain damage is severe.
Hypothermia treatment should also not be used when an infant demonstrates signs of mild hypoxic ischemic encephalopathy. It’s important that the diagnosis of HIE correctly assesses whether the condition is mild, moderate, or severe.

Re-Warming for Babies After a Cooling Treatment for HIE
A successful outcome after cooling depends on following proper protocol while re-warming the infant. After cooling, medical staff must carefully follow guidelines for re-warming.
Re-warming must occur over a minimum period of four hours. The ideal target is seven hours, at which point the infant’s temperature should reach 97.7 degrees Fahrenheit.
During re-warming, the infant’s temperature is incrementally increased by 0.9 degrees Celsius. A rectal temperature probe should be used to accurately monitor the infant’s temperature throughout the re-warming process.
Re-warming requires a high level of monitoring. Throughout re-warming, a doctor should monitor:
Rectal temperature
Heart rate
Respiratory rate
Oxygen saturation
Blood pressure
Once the target body temperature has been reached, the infant may undergo a variety of lab work for further monitoring. The re-warming process will necessarily induce bodily changes. Re-warming might trigger:
- Increased heart rate
- Decreased blood pressure
- Decreased urine output
- Imbalanced electrolytes
Failure to provide careful monitoring and sufficient re-warming time can result in brain injury and other serious consequences such as reperfusion injury — tissue damage that results from the blood supply being restored to the area too quickly.
What Happens After Hypothermia Treatment for HIE?
Infants must be carefully monitored during and after the re-warming process. The use of ECG monitoring is particularly useful, as re-warming can increase the risk of seizures. After hypothermia treatment, medical providers must watch for reperfusion injury.
Reperfusion is the process of restoring blood flow to tissues or an organ. In the case of hypothermia treatment for HIE, blood flow is restored to the infant’s entire body. During this process, reperfusion to the infant’s brain is of particular concern, as reperfusion injury is a risk. If this happens, then further brain damage is a possibility.
Reperfusion is a complex process. Although it’s necessary to restore blood flow to tissues in order to save them, the process can also result in extensive tissue destruction, especially if blood flow is restored too quickly. Carefully following re-warming guidelines and aiming for the target re-warming time of seven hours can reduce this risk.
After re-warming is complete, monitoring should include:
- MRI imaging of the brain
- Cardiovascular and respiratory systems
- Regular eating and diaper output
- Developmental signs, such as sucking and body movements.
Overall prognosis after cooling therapy is complete will be determined over time. Outcomes will vary by the degree of brain damage that occurred at birth and any other complications that might impact an infant’s health.
Benefits of Cooling Treatments for HIE
Clinical trials have shown that therapeutic hypothermia is a safe treatment option for infants at risk of HIE and can reduce the likelihood of death or brain damage.
One study compared the outcomes for 1,440 infants divided between a control group and a hypothermia group and found that cooling treatment resulted in a significant reduction of mortality risk, brain damage, and other developmental problems by 12 months of age.

Another retrospective study monitored 208 infants born with HIE. The team of researchers conducted follow-ups with families after six or seven years. The authors of the study found that children in the hypothermia group had a mortality rate of only 28%, a significant reduction compared with the control group’s mortality rate of 44%.
Recent research builds upon early studies, continuing to show improved outcomes for infants who received cooling therapy for HIE. The information available from clinical trials confirms that hypothermia treatment plays an active role in reducing the following:
- Mortality rate
- Neurodevelopmental delay and disability
- Cerebral palsy
- Cognitive delay
- Psychomotor delay
- Severe visual deficit
Cooling therapy is a relatively new treatment. It is still considered experimental, and further studies are needed to assess its long-term effects. Studies into the potential for hypothermia therapy began only 25 years ago, and conclusive study results have made the therapy more widespread since 2005.
Although there’s enough research on therapeutic hypothermia that it has become the standard of care, it’s important to recognize that cooling therapy is a relatively new treatment, and could still be considered experimental. Further studies are needed to assess its long-term effects. Studies into the potential for hypothermia therapy began only 25 years ago, and conclusive study results have made the therapy more widespread since 2005. Researchers are still learning more about how to optimize the use of this therapy to provide the best possible effects.
Risks of Cooling Treatments for HIE
Cooling can still be considered an experimental medical treatment for HIE, and it is not without risks.
Infants being treated for HIE have already suffered a serious birth injury. Extended induced hypothermia can cause additional adverse events. While hypothermia therapy is in progress, supportive treatment may be necessary.
Common additional support measures include:
- Respiratory support
- Cardiovascular support
- Positioning and skincare
- Feeding
- Sedation
- Coagulation
- Medication
An infant undergoing cooling therapy may also need monitoring and support with fluid and electrolyte imbalance, especially:
- Sodium
- Chloride
- Magnesium
- Calcium
- Glucose
Cooling treatment may increase the risk of reperfusion injuries such as brain swelling (edema) or brain tissue death during the re-warming process.
Other experimental treatments are still being explored for improving the treatment and prognosis of infants diagnosed with HIE.
Some alternative options to cooling therapy are available for general information purposes through the Cochrane website. Cochrane is an international organization that reviews and collects health care information to help people make informed decisions about their health. As an independent third-party organization, Cochrane takes into account the quality of the scientific studies it reviews, and offers trustworthy medical advice. Anyone can search for research-based reviews on medical treatments using the Cochrane database.
Cochrane review is an indication that a study was conducted according to the highest standards and offers trustworthy medical advice. The Cochrane site provides answers to questions about experimental alternatives to hypothermia treatment, such as:
- Acupuncture
- Inhaled xenon with cooling
- Erythropoietin (EPO)
- Stem cell-based therapies
When an infant does not meet the criteria for cooling therapy, another experimental treatment may extend their lifespan and reduce the degree of disability they experience.
Common Side Effects
Clinical studies have shown that cooling therapy is generally safe and poses few risks when the protocol is followed correctly and the infant is monitored carefully during and after therapy.
Potential side effects during treatment include:
- Sinus bradycardia (slowed heartbeat)
- Sepsis
- Pneumonia
- Thrombocytopenia (low platelets)
These side effects pose a low risk when compared with the potential for cooling therapy to lower infant mortality and reduce the severity of brain damage and other complications of HIE.
HIE is one of the leading causes of infant death. There are many reasons why an infant might be born with HIE. Possible causes include the position of the umbilical cord, untreated medical conditions in the mother, and prolonged labor. Unfortunately, these issues sometimes occur due to medical malpractice.
If your child was treated with cooling therapy after birth, you could benefit from speaking with a Hypoxic ischemic encephalopathy attorney about whether your child’s birth injury was the result of a preventable instance of medical negligence. Procuring legal advice is the first step in assessing whether you qualify for compensation after medical malpractice has caused serious injury.
Contact the team at Birth Injury Center to schedule a free consultation for legal assistance if you think your child’s hypoxic-ischemic encephalopathy, and the resulting need for treatments like cooling therapy, may have been the result of medical negligence.
Written by:
Birth Injury Center Team
The Birth Injury Center aims to create informational web content and guides to help women and their families seeking support and guidance for birth injuries caused by medical negligence. All of the content published across The Birth Injury Center website has been thoroughly investigated and approved by medical expert Natalie Speer, RNC-OB.

